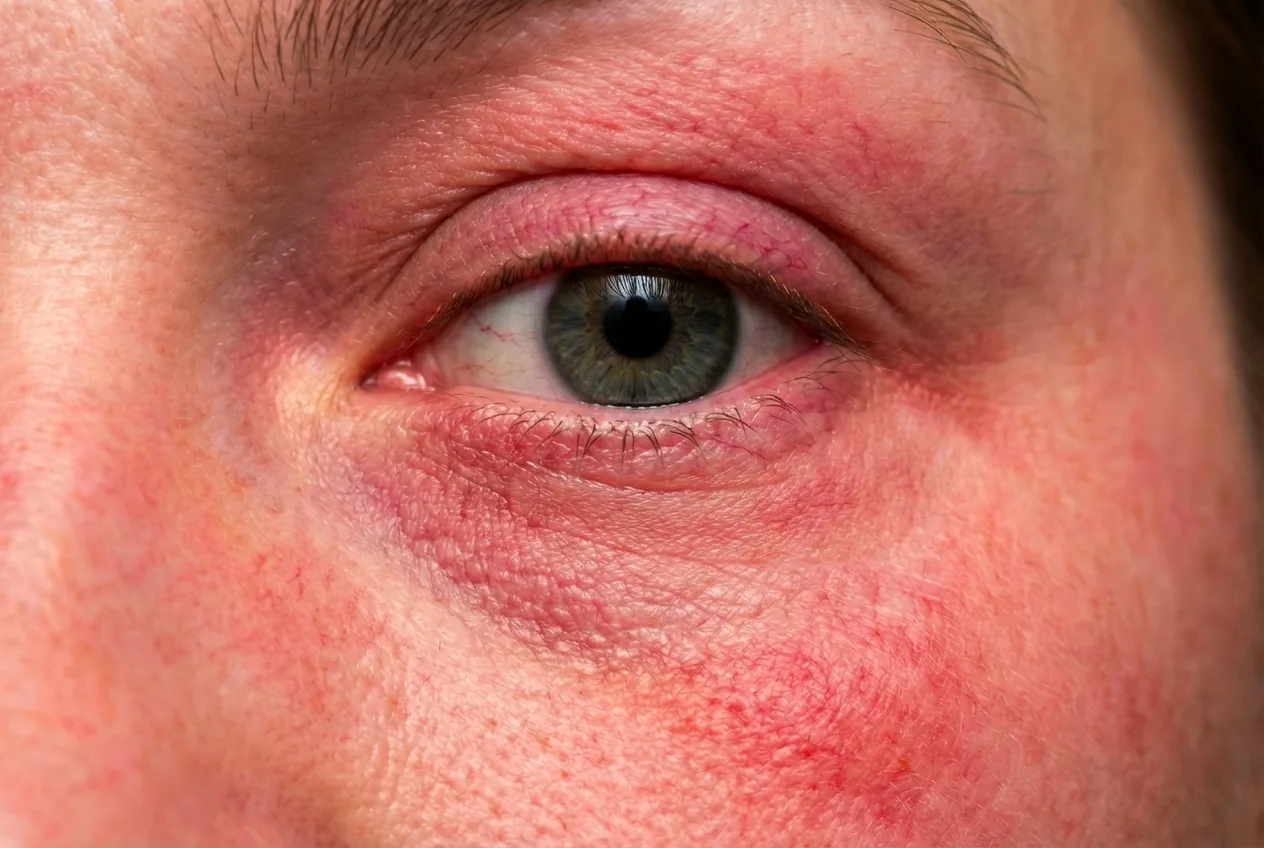
Rosacea is a common skin condition that manifests as redness, mid-facial flushing, swelling, prominent vasculature and papules or pustules. So what is ocular rosacea? This eye condition is a type of rosacea that causes inflammation, redness, itching and burning of the front of the eye and the eyelids.
Ocular rosacea also includes:
- Conjunctival hyperaemia, where blood flow increases to the eyes.
- Blepharitis is a common eyelid disease characterised by thickening, redness, flaky and scaly crusting of the eyelashes and eyelids. Blepharitis is also referred to as “eye dandruff”.
- Rosacea-associated keratitis is a complication of acne rosacea, where the skin becomes flushed before nodules and pustules form.
strong>Ocular rosacea is a chronic eye disease that has no cure. However, there are treatments available that can relieve symptoms. Read on to discover the symptoms of ocular rosacea, what causes ocular rosacea flare-ups, and how to treat ocular rosacea.
Are you experiencing symptoms of ocular rosacea?
The signs and symptoms of ocular rosacea can include:
- Red, inflamed, or swollen eyelids, particularly at the base of the eyelashes.
- Itching, burning, or watering eyes.
- Feeling like there is something stuck in the eyes.
- Discolouration around your eyes.
- Dry eyes.
- Crusty discharge in your eyelashes.
- Formation of chalazion, a slow-developing lump that forms because of an oil gland swelling or being blocked in the eyelids.
- You have clogged oil glands in your eyelids.
- Recurring styes. These painful red bumps can form near the eyelid edge and appear like a pimple or boil.
- Sensitivity to light.
Who commonly experiences ocular rosacea?
Ocular rosacea can affect all types of people. However, some groups of people are more prone to developing this eye condition, including:
- Women and people who are assigned female at birth.
- People with fair or light skin.
- For adults between 30 and 50 years of age, it is uncommon in children.
- People with a Western European ethnic background, mainly from Scotland or England.
While ocular rosacea usually occurs in people who have facial flushing, it can also be the first sign a person has rosacea that has not been diagnosed yet.
What causes ocular rosacea flare-ups?
Rosacea is a skin condition that is non-contagious and typically affects the face. Featuring inflammation, a permanent flush, enlarged capillaries, and non-tender pustules, the exact cause of rosacea and ocular rosacea is unknown.
Research has indicated a possible link between the helicobacter pylori bacteria (the bacteria that causes gastrointestinal infections) and rosacea. Other research shows it is caused by tiny mites or organisms that block oil glands, resulting in a swollen and red face. The Demodex mites live on your eyelashes and are a part of your skin’s normal flora, but they can stimulate inflammation, which causes ocular rosacea to develop.
Other research indicates immunological factors, reactive blood vessels and micro-organisms on the skin surface are involved in developing ocular rosacea. A positive family history can sometimes indicate the prevalence of ocular rosacea development.
Once you can identify what triggers an ocular rosacea flare-up, you may be able to avoid them. Common triggers of Ocular rosacea flare-ups can include:
- Hot drinks
- Spicy foods
- Hot baths or saunas
- Caffeine
- Chocolate
- Drinking alcohol
- Experiencing intense temperatures of the sun or wind
- Some drugs like cortisone or vasodilating medications
- Feeling angry, embarrassed, or stressed.
Can you cure ocular rosacea completely?
There is no complete cure for ocular rosacea. However, there are treatments that can control the signs and symptoms. As a chronic, long-term eye condition, ocular rosacea can be managed by understanding your genetic predispositions and what your triggers are. Find out how to treat ocular rosacea below.
If you have ocular rosacea, you should visit an eye doctor regularly so they can evaluate your corneas and assess if the treatments are beneficial. Ocular rosacea treatments typically include:
- Eye drops or steroid drops to reduce swelling and redness.
- Antibiotic ointments or medications to treat eye infections.
- Eyelid scrubs to keep your eyes infection-free and clean.
- Artificial tears to keep your eyes moist.
It is important to note that if left untreated, ocular rosacea can affect the cornea, resulting in it becoming inflamed and damaged. This can lead to infections that could affect eyesight.
Fast, short-term treatments for ocular rosacea
A step-by-step approach must be taken under your doctor’s guidance when treating ocular rosacea. Treatment usually starts with lid hygiene, where warm compresses are applied to the eyelids to help liquefy the secretions. Mild, non-irritating cleaning solutions your doctor suggests must be used to remove any clogged debris.
Next, you may need to use artificial tears throughout the day. Sometimes, you may also need to apply a lubricating ointment at night. Some of these ointments contain antibiotics.
If artificial tears are not giving you the required results, you may need twice-daily applications of topical cyclosporine. This medication has proved more efficacious than artificial tears to manage ocular rosacea.
It is common to treat ocular rosacea with antibiotics, with the most popular being tetracycline, doxycycline, and minocycline.
To provide short-term relief for the lid disease and the management of inflammatory keratitis, topical treatments can be used, including steroids. Long-term use of steroids can exacerbate ocular rosacea, though.
Retinoids (Vitamin A derivatives), anti-ulcer therapy, and topical acne treatments, including azelaic acid and Ivermectin, may also be prescribed for treatment.
How long does ocular rosacea last
Ocular rosacea is a chronic, long-term condition with no known cure. It can be managed by avoiding your triggers and undertaking treatments prescribed by your doctor. Once diagnosed with ocular rosacea, it may take weeks or months of treatment before you notice any significant improvement in symptoms.
Sometimes, you may need to combine different treatments to get the best outcome for your condition.
Can I prevent ocular rosacea flare-ups from happening?
While you can do nothing to prevent ocular rosacea, you can manage symptoms and avoid triggers as much as possible. Other ways to prevent flare-ups include:
- Avoid your triggers as much as possible.
- Keep your eyelids clean by gently washing and drying them. If necessary, use the cleaning product as directed by your doctor.
- Avoid wearing contact lenses during a flare-up. This is particularly important if you also have dry eyes.
- Under the guidance of your doctor, use artificial tears to prevent dry eyes.
- Avoid wearing make-up during a flare-up.
When should I see my healthcare provider?
If your ocular rosacea symptoms worsen or your flare-ups happen more frequently, you should make an appointment with your healthcare provider. If you experience new symptoms or triggers, you should also see them.
If you have itchy, burning, or red eyes, seeing a doctor as soon as possible is essential.
You must go to an emergency room if you have intense pain, dizziness, loss of vision or blurry, double vision. Delaying treatment may cause irreparable damage.
What questions should I ask my doctor about ocular rosacea?
The first step to diagnosing ocular rosacea is to visit your general medical doctor. Treating ocular rosacea is a life-long journey. At your doctor’s appointment, make sure you ask the following questions.
What treatments do I need?
The treatments you need will depend on the extent of your ocular rosacea. Eye doctors with experience in diagnosing and treating this eye condition can prescribe the correct treatment for your condition. This could involve applying eye compresses, eye drops, or oral medication.
Will I need any medicines?
Each case of ocular rosacea is different. Your condition will differ from others, so an in-depth consultation with a specialist eye doctor or dermatologist is needed.
Do I need to see a specialist?
Your doctor may refer you to an eye specialist with experience in ocular rosacea. If you have rosacea and are under a dermatologist’s care, they can work with the eye specialist to develop a treatment plan.
What activities, foods or drinks should I avoid?
Learning what triggers the ocular rosacea can take a while. Your doctor may suggest that you diarise about what you eat and drink, how stressed you are, or if you are too warm or cold. These factors can all contribute to an ocular rosacea flare-up. Once you know your triggers, you can avoid them as much as possible.
Come down and see one of our eye doctors in Kennesaw or East Cobb today
Do you think you have ocular rosacea? It’s essential to seek out a doctor if you develop eye issues to avoid potential problems with vision. Some people with ocular rosacea experience issues with the cornea, which can affect their ability to see. Please book an appointment with our doctors today.